Her hands permanently stained by other people’s lives.
Her back bent from years of labor that started before dawn and ended after dark.
Isabelle’s nursing program had been funded by remittances from an aunt working in Dubai.
Payments that came with the unspoken understanding that success wasn’t optional.
The pressure to excel, to escape, to lift her family from poverty had shaped every decision she had made since childhood.
When the opportunity arose to work in Singapore, she didn’t hesitate despite knowing it meant leaving behind everything familiar.
Her HDB flat in Angokio was a world away from the luxury of her patients lives.
She shared the three- room apartment with three other Filipino nurses.
Grace, who worked in pediatrics, Maria, who specialized in geriatrics, and Carmen, who had been in Singapore for seven years and served as their unofficial mentor in navigating both the health care system and the complex social dynamics of being foreign workers in one of the world’s most expensive cities.
Each of them was sending money home.
Each of them carried the weight of family expectations that stretched across thousands of miles.
Each of them understood the delicate balance between gratitude for opportunities and homesickness for everything they had left behind.
The apartment was clean but cramped, filled with the smell of cooking rice and the sound of video calls home during precious off hours.
Every month, Isabelle sent $800 to her parents.
Money that paid for her youngest sister’s university tuition, her brother’s medical school prerequisites, and the small improvements that gradually lifted their standard of living.
The wire transfer receipts were filed carefully in a shoe box under her bed.
Tangible proof of progress toward dreams that sometimes felt impossibly distant.
At Mount Elizabeth Hospital, Isabelle had quickly established herself as someone special.
Patients requested her specifically.
Families thanked her personally.
Colleagues relied on her during crisis situations.
She possessed the rare combination of clinical competence and emotional intelligence that made people feel safe in her presence.
Her English was excellent, flavored with the gentle accent that reminded patients of the Filipina nurses they had encountered throughout Southeast Asia’s medical facilities.
The infectious disease ward was particularly demanding.
Patients arrived frightened, often facing diagnoses that carried social stigma along with medical consequences.
HIV positive patients especially required not just clinical care but emotional support as they navigated treatment protocols and family dynamics that could range from supportive to completely rejecting.
Isabelle excelled in this environment because she understood what it meant to carry burdens that couldn’t be shared to smile through pain to maintain hope when circumstances seemed hopeless.
When a young businessman broke down after testing positive for HIV, convinced his life was over, Isabelle didn’t just offer medical facts.
She sat with him through the night, holding his hand while he grieved the future he thought he was losing, helping him understand that diagnosis wasn’t destiny.
My cousin back home has been HIV positive for 8 years, she told him quietly.
He’s married now, has two beautiful children, runs a successful business.
The medicine today is like managing diabetes.
It’s not easy, but it’s manageable.
Her supervisor, nurse manager Patricia Wong, had noticed Isabelle’s exceptional patient rapport within weeks of her arrival.
She has something special, Patricia noted in Isabelle’s performance review.
Patients calm down when she enters the room.
families trust her completely, and her clinical knowledge is impressive for someone with her experience level.
What Patricia didn’t know was that Isabelle’s knowledge came from hours of additional study, research papers downloaded, and read during her commute, medical journals borrowed from the hospital library.
She was driven not just by professional ambition, but by a genuine desire to understand the science behind the suffering she witnessed daily.
that dedication would soon catch the attention of someone whose notice would change her life forever.
It was during one of these difficult cases on a humid Thursday evening in October that Dr. Marcus Tan first truly noticed Isabelle Cruz.
And in that moment of professional recognition, the countdown to catastrophe began.
The patient was a 24year-old expatriate teacher named David Chun who had tested positive for HIV after a routine health screening required for his work visa renewal.
The young man was inconsolable, convinced that his life was over, that his family would disown him, that he would die alone and in shame.
Three different doctors had tried to calm him, explaining treatment protocols and prognosis statistics with the clinical detachment that medical training demanded, but he remained hysterical, his sobs echoing through the infectious disease wards usually subdued corridors.
Marcus was reviewing the case notes in his office when he heard something that made him pause.
gentle singing in Tagalog accompanied by the kind of quiet conversation that suggested someone was actually listening rather than just talking.
The melody was unfamiliar but soothing, threading through the antiseptic atmosphere like incense in a cathedral.
Curious, he made his way to room 712, where he found Isabelle sitting beside David’s bed, her hand resting lightly on his shoulder, explaining HIV treatment in terms that acknowledged both the medical realities and the emotional devastation.
The medicine has come so far.
She was saying her voice carrying the kind of authority that comes from genuine knowledge rather than memorized protocols.
With proper treatment, people with HIV live normal lifespans.
They have families, careers, full lives.
This isn’t the end of your story, David.
It’s just a different chapter, and you get to decide how that chapter unfolds.
What struck Marcus wasn’t just her compassion, though that was evident in every gesture.
It was her clinical knowledge.
She was discussing viral load counts, medication interactions, and resistance patterns at a level that impressed him.
When she explained how modern anti-retroviral therapy worked, she used analogies that made complex immunology accessible without being condescending.
When she addressed David’s fears about transmission and relationships, she combined medical facts with genuine empathy in ways that Marcus rarely witnessed from nursing staff.
Dr. Tan is our chief of infectious diseases.
She told David when she noticed Marcus standing in the doorway.
He’s one of the leading HIV researchers in Southeast Asia.
You’re in the best possible hands.
Marcus found himself engaging with the patient differently because of Isabelle’s presence.
Her questions were insightful, revealing understanding that went beyond basic nursing protocols.
Her observations about patient psychology were accurate and nuanced.
Her suggestions for treatment approaches demonstrated comprehension of not just the medical aspects but the social and emotional complexities that could affect treatment compliance.
Have you considered the psychological impact of the medication schedule on younger patients?
She asked Marcus during their discussion.
In my experience, patients David’s age struggle more with the routine than the actual side effects.
They feel like the medication schedule makes their condition visible to roommates and friends.
It was an astute observation that Marcus hadn’t fully considered.
Most of his focus remained on viral suppression and drug resistance.
The social implications of treatment regimens were typically left to social workers and counselors.
But Isabelle was identifying a real barrier to treatment compliance that could affect long-term outcomes.
After they left David’s room, Marcus lingered in the corridor.
The shift change was still 2 hours away, but most of the day staff had already departed, leaving the ward in the quieter rhythm of evening care.
“You handled that beautifully,” he said genuinely impressed.
“Where did you develop such comprehensive HIV knowledge?
I’ve always been interested in infectious diseases,” Isabelle replied, her professional demeanor remaining intact despite the compliment from such a senior physician.
I actually read your recent paper on drugresistant HIV strains in Southeast Asian populations.
The implications for treatment protocols were fascinating, especially the resistance patterns you identified in patients with incomplete treatment histories.
Marcus was genuinely surprised.
His research was highly specialized, published in journals that most nursing staff wouldn’t encounter in their routine professional development.
The fact that she had not only read it but understood its clinical implications suggested an intellectual curiosity that went far beyond job requirements.
“What did you think about the correlation between socioeconomic factors and resistance development”?
he asked, testing the depth of her understanding.
The conversation that followed lasted 25 minutes and covered territory that Marcus typically only explored with fellow physicians and research collaborators.
Isabelle asked questions that revealed not just curiosity but genuine understanding of complex medical concepts.
She shared observations from her patient interactions that provided insights Marcus hadn’t considered, particularly regarding how cultural factors influence treatment adherence among Southeast Asian immigrant populations.
In my experience, she said, patients from traditional families often struggle with disclosure issues that affect their support systems.
They might have excellent medical care here, but if they can’t explain their medication schedules to family members without risking social isolation, compliance becomes much more difficult.
It was the kind of observation that could influence policy decisions, the type of insight that came from combining clinical knowledge with real world cultural understanding.
By the time they parted ways, Marcus was looking at Isabelle Cruz very differently than he had that morning.
Over the following weeks, Marcus found excuses to consult with Isabelle on difficult cases.
He began requesting her for his most challenging patients, justifying the assignment by pointing to her exceptional rapport with HIV positive clients and her demonstrated understanding of complex treatment protocols.
Their professional interactions gradually extended beyond immediate medical needs.
They discussed research papers over coffee in the hospital cafeteria.
They debated treatment approaches during quiet moments between patient rounds.
“Have you ever considered pursuing additional certification in infectious disease nursing”?
Marcus asked during one of their coffee conversations in November.
“Your clinical insight is remarkable.
You could easily qualify for specialized programs”.
Isabelle was flattered by the attention from such a distinguished physician.
Marcus was 15 years her senior, internationally respected, the kind of doctor whose opinion could open doors throughout the medical world.
When he asked for her thoughts on complex cases, when he shared insights from his research, when he treated her as an intellectual equal rather than just another nurse following orders, she felt valued in ways she had rarely experienced.
I’ve thought about it, she admitted, but the programs are expensive and I have family obligations back home.
Maybe someday when my siblings finish school.
The hospital has continuing education grants, Marcus suggested.
I could recommend you for consideration.
Your work deserves recognition.
These conversations revealed more than professional respect.
Marcus learned about Isabelle’s family responsibilities, her financial pressures, her dreams of advancement that seemed perpetually deferred by circumstances beyond her control.
She learned about his research passions, his frustrations with hospital politics, his genuine dedication to advancing HIV care in the region.
The transition from professional collaboration to personal intimacy began during a particularly difficult night shift in late November.
They were treating Maria Santos, a young mother who had unknowingly transmitted HIV to her newborn during childbirth.
The baby’s prognosis was uncertain, and Maria’s guilt was overwhelming every medical intervention they attempted.
She blamed herself not just for her child’s infection, but for her own positive status, which she had discovered only during prenatal testing.
I should have known.
Maria kept repeating through tears.
I should have protected my baby.
What kind of mother doesn’t protect her baby?
For six hours, Marcus and Isabelle worked together to stabilize the infant while providing emotional support to a mother whose grief threatened to interfere with the medical care both she and her baby required.
The case required not just clinical expertise, but psychological finesse, cultural sensitivity, and the kind of emotional endurance that few healthcare providers could sustain indefinitely.
After the baby was finally stable and Maria had been sedated for desperately needed rest, Marcus and Isabelle found themselves alone in his office at 3:00 a.
m.
Exhausted and emotionally drained.
The usual professional boundaries felt less relevant after sharing such an intense experience.
“Sometimes I wonder if we’re actually helping people or just prolonging their suffering,” Marcus said, his usual confidence replaced by rare vulnerability.
The question hung in the air between them, heavy with implications about the nature of their work and the limits of medical intervention.
You helped Maria understand that love doesn’t stop because of a diagnosis, Isabelle replied thoughtfully.
You gave her hope that her baby can still have a beautiful life.
That’s not prolonging suffering.
That’s creating possibility where she saw only despair.
Do you really believe that?
That hope is always justified.
Isabelle considered the question seriously, recognizing that Marcus was asking something deeper than professional philosophy.
I think hope is all we have sometimes.
In my family, when my father had his accident and couldn’t work for 6 months, hope was what kept us from giving up.
Hope that things would get better, that sacrifices would lead to something meaningful.
Marcus found himself sharing details about his own life that he rarely discussed with colleagues.
The pressure of maintaining his reputation in Singapore’s small medical community.
The weight of life and death decisions that followed him home every night.
The isolation that came with being seen as infallible when he often felt like he was improvising solutions to problems that had no clear answers.
Jennifer doesn’t understand the emotional toll.
He admitted the words emerging before he fully considered their implications.
She sees the prestige, the income, the social status, but she doesn’t see what it costs to be responsible for so many lives, to make decisions where being wrong means someone doesn’t go home to their family.
Isabelle listened without judgment, offering insights that revealed her own depth and emotional intelligence.
She understood family pressure, professional expectations, the burden of being someone others depended on for their survival and well-being.
Their conversation lasted until dawn, creating an intimacy that transcended their professional relationship and planted seeds that would grow into something much more dangerous.
The first time they kissed was 3 weeks later in an empty consultation room after losing a patient to complications from AIDS related pneumonia.
They had fought for hours to save Chun Wei Ming, a 35-year-old father of three who had responded well to treatment until a sudden respiratory crisis overwhelmed his compromised immune system.
The family’s grief was devastating.
Their gratitude mixed with desperate hope that somehow the doctors could still perform a miracle.
Weings wife had collapsed against the wall when Marcus delivered the news.
Her sobs echoing through corridors where death was supposed to be managed with quiet dignity.
Their children, aged 8, 10, and 12, stood in bewildered silence, too young to fully understand that their father was gone, but old enough to recognize that their world had just shattered.
In the aftermath, as they cleaned up the medical equipment and completed the necessary documentation, Marcus and Isabelle found themselves standing close together, sharing the weight of failure that every health care provider knows intimately.
When Marcus reached out to comfort her, when his hand touched her shoulder and she looked up at him with tears reflecting their shared grief, the kiss happened with an inevitability that neither of them questioned in that moment.
“We shouldn’t,” Isabelle whispered, even as she didn’t pull away from his touch.
“I know,” Marcus replied, his forehead resting against hers.
“But I can’t stop thinking about you”.
The admission hung between them like a diagnosis that would change everything.
In that sterile room where they had just witnessed the limits of their professional power, they found something that felt infinite and dangerous and completely beyond their control.
The affair was about to begin in earnest, and with it, the countdown to catastrophe that would destroy not just their own lives, but the lives of everyone who trusted them.
The affair escalated quickly after that first kiss in the consultation room.
Marcus rented a service department in River Valley under the name Michael Lim, paying cash for a year-long lease that provided them with privacy away from the hospital’s watchful eyes and Singapore’s interconnected social circles.
The apartment was on the 28th floor of a luxury complex, modern and anonymous with floor toseeiling windows that overlooked the Singapore River’s gentle curve through the heart of the city.
It was furnished with the kind of sterile elegance found in upscale hotels, neutral colors, expensive materials, and absolutely no personal touches that might suggest permanence.
Their Wednesday evening meetings became sacred time carefully choreographed around Marcus’ family obligations and Isabelle’s work schedule.
Marcus would tell Jennifer he was attending medical conferences or consulting on complex cases that required extended evening hours.
The lies came easily, supported by his reputation for dedication and the demanding nature of his specialization.
Jennifer, absorbed in her own career pressures and the logistics of managing their household, rarely questioned his absences.
Isabelle would arrange her schedule to ensure she was available, often trading shifts with colleagues who assumed she was simply trying to pick up extra hours for the overtime pay.
Her roommates in the Ang Moio flat grew accustomed to her Wednesday evening disappearances, attributing them to the demanding social expectations of working with Singapore’s medical elite.
In that apartment, they created a bubble separate from their real lives where Marcus could be vulnerable and Isabelle could feel cherished in ways that transcended anything she had experienced before.
Marcus was an attentive lover, someone who understood that seduction involved emotional as well as physical intimacy.
| Continue reading…. | ||
| « Prev | Next » | |
News
MEL GIBSON UNCOVERS HIDDEN TRUTHS ABOUT JESUS FROM AN ANCIENT BIBLE!!! In a groundbreaking cinematic endeavor, Mel Gibson is set to challenge the very foundations of Western Christianity with his upcoming film, “The Resurrection of the Christ,” which promises to reveal a side of Jesus that has been deliberately obscured for centuries. Drawing inspiration from the Ethiopian Orthodox Bible and the enigmatic Book of Enoch, Gibson’s narrative will transport audiences through realms unknown, exploring not only the resurrection but also the fall of angels and the cosmic battle between good and evil. As production ramps up in Rome, the film aims to intertwine ancient scripture with a bold vision that defies traditional storytelling. What lies within the pages of the Ethiopian texts could shatter long-held beliefs, portraying Christ not merely as a gentle savior but as a powerful, overwhelming force with the authority to command both angels and demons. With a release date set for Good Friday 2027, the stakes are high—will this film awaken a new understanding of faith, or will it provoke a backlash that echoes through history? The question remains: what else has been buried, and who will be ready to confront the truth?
The gods have throne guardians. This is a rare Ethiopian Orthodox Bible manuscript. The Book of Enoch is part of the literature that’s trying to explain that. Right now, Mel Gibson is at Cinita Studios in Rome, building what he calls the most important film of his life. And the version of Jesus Christ he […]
GENE HACKMAN’S SECRET TUNNEL: A DISTURBING DISCOVERY REVEALED!!! In a shocking turn of events, the death of legendary actor Gene Hackman and his wife Betsy has unveiled a chilling mystery hidden beneath their Santa Fe estate. After authorities forced entry into their secluded compound, they discovered not only the couple’s bodies but also a concealed tunnel leading to an underground chamber filled with bizarre artifacts and coded documents. As the FBI investigates, the unsettling timeline raises questions: why did Hackman remain silent for a week with his deceased wife, and what dark secrets were buried within the walls of his home? The agents’ findings suggest a life shrouded in secrecy, with markings and inscriptions hinting at a history far more sinister than anyone could have imagined. With an iron door sealed from within, the question looms—what lies behind that door, and why has the FBI kept it hidden from the public? This is a story that could change everything we thought we knew about one of Hollywood’s most private figures
Tonight, we’re learning new details in the death of legendary actor Gan Hackman. Deaths of Oscar-winning actor Gan Hackman and his wife, whose bodies were found in their Santa Fe home. 1425 Old Sunset Trail, where Gene Hackman, 95, and his wife Betsy Arakawa, 65, and a dog were found deceased. 40t below Gene Hackman’s […]
A TIME MACHINE BUILT IN A GARAGE: THE MYSTERIOUS RETURN OF MIKE MARKHAM!!! In a chilling tale of obsession and discovery, self-taught inventor Mike Markham vanished without a trace in 1997 after claiming to have built a time machine in his garage. As the world speculated about his fate—ranging from time travel to government abduction—Markham’s story became an internet legend. After 29 years, he reemerges, older and weary, carrying a box filled with journals and evidence of his experiments, but what he brings back is not the proof of time travel everyone hoped for; it’s something far more sinister. As he recounts his journey from rural tinkerer to a man on the brink of a new reality, the question looms: what horrors did he encounter during his years away, and what dark secrets lie within the technology he created? With each revelation, the line between reality and the unimaginable blurs, leaving audiences to wonder—has he truly returned, or has he brought something back that should have remained lost in time?
Back to the future. Could it actually happen with a real time machine? I was devastated. I thought if I could build a time machine that I could go back and see him again and tell him what was going to happen, maybe save his life. And so that became an obsession for me. In […]
MEL GIBSON REVEALS SHOCKING SECRETS ABOUT THE PASSION OF THE CHRIST!!! In a jaw-dropping interview on the Joe Rogan podcast, Mel Gibson pulls back the curtain on the making of The Passion of the Christ, exposing hidden truths that could change everything we thought we knew about this controversial film. As Gibson recounts the extraordinary resistance he faced from Hollywood, he reveals how the industry’s skepticism towards Christian narratives nearly derailed the project altogether. With insights into the film’s raw and visceral storytelling, Gibson reflects on the spiritual warfare depicted in every scene, challenging audiences to confront their own beliefs about sacrifice and redemption. But as he hints at supernatural occurrences on set and the profound transformations experienced by cast members, a chilling question arises: what deeper truths lie beneath the surface of this cinematic masterpiece, and how will Gibson’s upcoming sequel reshape our understanding of faith and history?
It was a great movie, but it seemed like there was resistance to that movie. Mel Gibson was on the Joe Rogan podcast talking about the sequel to The Passion of the Christ. What if the most controversial film of the century contained secrets that nobody was meant to discover? When Mel Gibson sat down […]
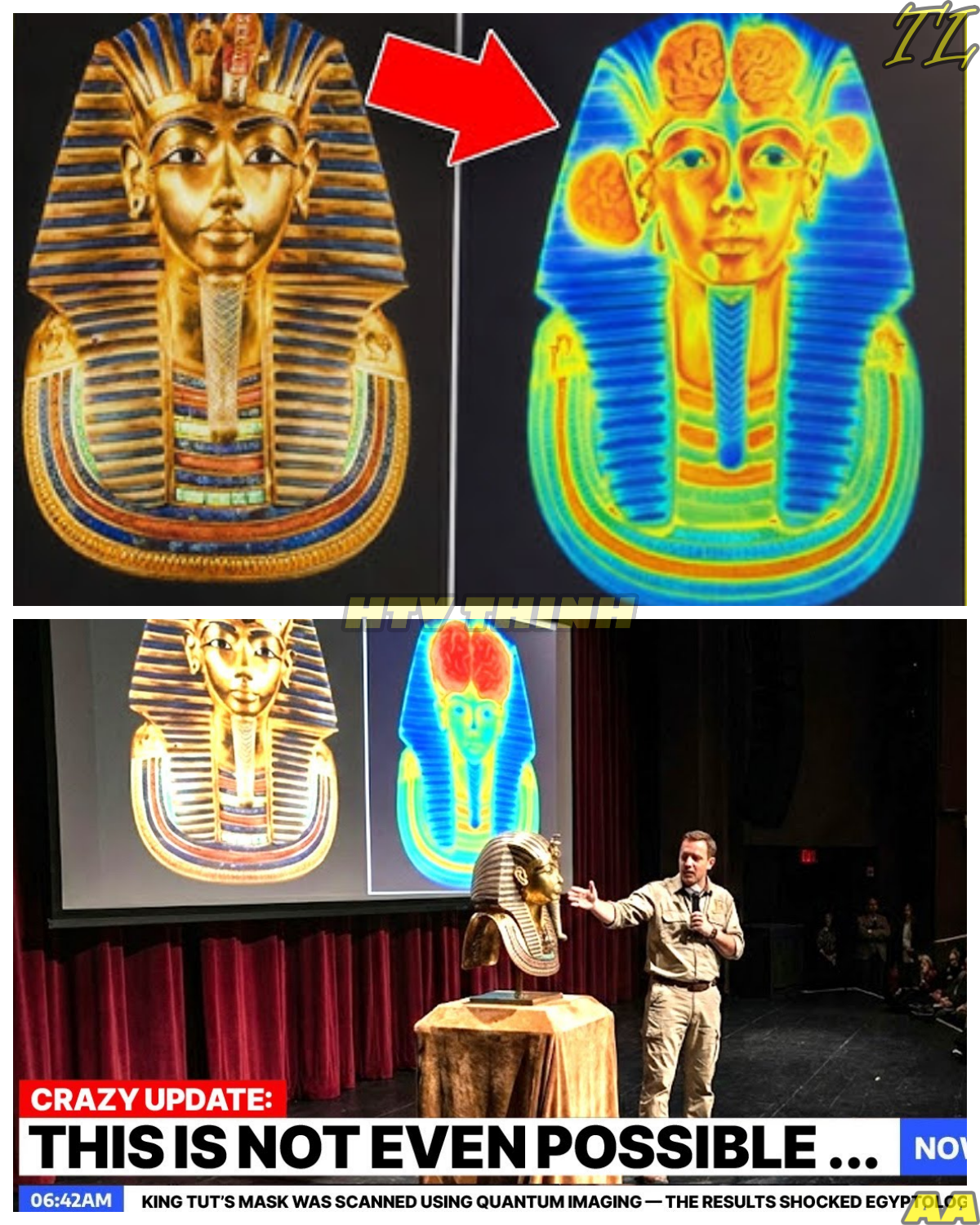
THE SHOCKING TRUTH BEHIND KING TUT’S MASK REVEALED AT LAST!!! In a groundbreaking revelation that could rewrite history, a team of physicists has employed cutting-edge quantum imaging technology to uncover a hidden truth about King Tutankhamun’s iconic death mask. For over 3,300 years, this 22-pound gold masterpiece has captivated the world, but new scans reveal a name beneath the surface that doesn’t belong to the boy king. As experts grapple with the implications of this discovery, they face a ticking clock—will the truth about the mask’s origins shatter the long-held beliefs of Egyptology? With whispers of a powerful queen whose legacy has been erased from history, the stakes are higher than ever. As the evidence mounts, a chilling question emerges: whose face was originally meant to adorn this sacred artifact, and what secrets lie buried in the sands of time?
Layers and layers and layers of information are coming out. Not just because objects are being um examined in detail, but also because new technologies can be applied to them. Was the mask created for Tuten Ammon or for someone else? For 3,300 years, the most famous face in history has been lying to us. […]
HAMAS DECLARES WAR: A NEW FRONT IN THE FIGHT FOR PALESTINE!!! In a chilling announcement from Gaza, Hamas’s military spokesperson, Abu Oda, has ignited a firestorm of tension across the Middle East, praising Hezbollah’s recent operations against Israeli forces and calling for intensified conflict. As Israel approves a controversial law permitting the execution of Palestinian prisoners, Abu Oda frames this moment as a pivotal turning point, highlighting the immense sacrifices of the Palestinian people and the silent genocide occurring in prisons. With a backdrop of escalating violence and deepening regional instability, he urges Arab and Muslim nations to take action against Israel’s aggression. As the stakes rise and the rhetoric hardens, the world watches with bated breath—will this conflict spiral into a wider war, drawing in more players and transforming the geopolitical landscape forever?
A new and explosive message is emerging from Gaza. The military spokesperson of Hamas al-Kasam brigades, the new Abu Oeda, has issued a fiery statement, one that is already sending shock waves across the region. In it, he praises Hezbollah’s recent operations against Israeli forces, calling them consequential and highlighting what he describes as heavy […]
End of content
No more pages to load